work: The sum of internal and external work?????
efficiency: The heart is more efficient when it can do more work with less of an increase of MVO2. Increasing the HR to increase CO is the lowest efficient way. The best way is to Increase SV by Starlings law (stretch). The next efficient way is to increase SV by contractility.
stroke work: External Work. About equal to SV * SBP
minute work: Stroke work * HR = SV * SBP * HR
internal cardiac work: Work done with no ejection of blood (Isovolumetric contraction)
external cardiac work: Work done during the ejection of blood.
myocardial oxygen consumption (MVO2): The amount of O2 used by the heart. During diastole the heart's MVO2 is about 15% of the total MVO2. The other 85% is during Contraction and Relaxation. As more work is done, the MVO2 increases.
rate-pressure product (RPP): An easy way to questimate the Minute work which is a good indicator of how much MVO2 is taking place is to find the product of HR and SBP. (MVO2 is about= HR * SBP)
myocardial wall tension:
Surface Tension Law: Law of LaPlace??? Tension = (Pressure * radius)/(wall thickness)
Pick equation for estimating coronary blood flow: ???????????????????
coronary sinus: Most of the venous blood flow from the left ventricle coronaries enters the right atrium by way of the coronary sinus, which is about 75% of the total coronary blood flow.
Thebesian vessels: A small amount of coronary blood flows back into the heart through minute thebesian veins, which empty directly into all chambers of the heart.
subendocardial plexus: Coronary vasculature of coronary arteries lying immediately beneath the endocardium. During systole, blood flow through the subendocardial plexus of the left ventricle, where the contractile force of the heart muscle is great, falls almost to zero. To compensate for this almost total lack of flow during systole, the subendocardial arterial plexus is more extensive than the nutrient arteries in the middle and outer layers of the heart. Therefore, during diastole, blood flow in the subendocardial arteries is considerably greater than is blood flow in the outermost arteries. Guyton page 257-258
cardiac nerves: For the most part, cardiac sympathetic stimulation of the nerves on the coronaries cause more vasoconstriction than dilation. For this reason the coronary blood flow is mostly controlled by metabolic needs.
autoregulation: Blood flow through the coronary system is regulated almost entirely by local arterial vasodilation in response to cardiac muscle need for nutrition....not neural stimulation.
adenosine: In the presence of very low concentrations of oxygen in the muscle cells, a large proportion of the cell's ATP degrades to adenosine monophosphate, then small portions of this are further degraded to release adenosine into the tissue fluids of the heart muscle. Adenosine is the substance with the greatest vasodilator propensity. Guyton 258
endothelin: Large peptide (21 amino acids). Present in endothelial cells of most blood vessels. Usually released upon damage to vessel walls. Constricts umbilical artery in newborn. Prevents bleeding after vessel injury. Prolonged vasoconstriction causes remodeling (+ vascular smooth muscle, + collagen, + elastin, + hypertrophy, - radius). Part of humoral autoregulatory response. Keeps tissue flow appropriate with changes in peripheral pressure.
myocardial ischemia: When the oxygen supply to the heart or an area of the heart is not enough to satisfy the oxygen demand.
demonstrate an understanding of the usefulness and appropriateness of the PRESSURE-VOLUME LOOP in estimating cardiac STROKE WORK: (This is from exam 1 notes)

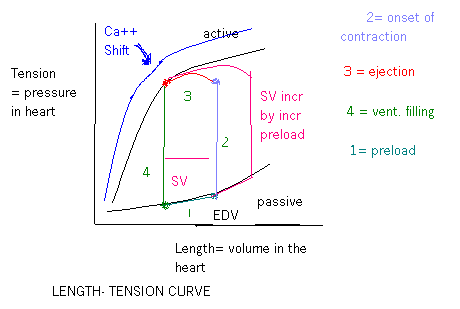
Any striated muscle as you stretch it, you bring actin and myosin crossbridges into an optimal alignment where the force generated is maximal. If you stretch them too much, you can’t form as many crossbridges and you have less contraction. Conversely, too little stretch and you physically limit the # of crossbridges you can form and you decrease contractile force. The optimal range of overlap or the active development of force is the isometric tension. You must stretch the heart by applying tension and the longer the stretch, the more tension applied to get it to that length and thus the greater contractile force. In the heart the factors that affect this force are the load applied to the muscle before it contracts and the load against which the muscle must work after it starts to contract or the preload and afterload. The diagram shows the pressure-volume loop. The end systolic volume (ESV) is the point in the corner of line 4 and line 1. The SV will be the difference between ESV and EDV. Preload will bring the heart to a certain EDV and the heart will begin to contract. The wall tension and pressure rises without any change in volume. When the ventricular pressure reaches a point where the aortic valve opens, volume will go down as it is ejected out. You can’t go past the line of shortening. It is the max force at this volume. The aortic valve closes and the vent relax – isovolumetric relaxation. Atrial pressures rise and the vent fill as the AV valves open.
demonstrate an understanding of the factors that contribute to MINUTE WORK of the heart, and compare and contrast the relative INCREASES IN MYOCARDIAL OXYGEN CONSUMPTION that occur when minute work is elevated because of: a) increased heart rate; b) increased stroke volume (increased preload); and c) increased afterload: Minute Work = (Stroke work * HR) = (SV * SBP * HR). The heart is more efficient when it can do more work with less of an increase of MVO2. Increasing the HR to increase CO is the lowest efficient way. The best way is to Increase SV by Starlings law (stretch/preload). This is the most efficient way. The next efficient way is to increase SV by contractility. The MVO2 of increased afterload is somewhere between SV by contractility and HR.
discuss the rate-pressure product (RPP) as a useful indicator of the level of MYOCARDIAL ENERGY UTILIZATION in some situations: If we increase minute work we increase myocardial energy use. Remember that minute work = (SV * SBP * HR). If we take the product of the SBP and HR (SBP * HR) at rest and compare it to the same product while a person is exercising you can get a good indicator to see how much the energy use has increased.
For example:
Rest--
SBP = 120
HR = 60
Product (120
* 60) = 7200
Exercising--
SBP = 160
HR = 180
Product (160
* 180) = 28800
Compare--
Exercising/Rest = 28800/7200 = 4
In the above example, the energy use of the heart has increased 4 times.
define PRELOAD and AFTERLOAD in terms of chamber radius, wall thickness, and chamber pressure as described in the Young-LaPlace Surface Tension Law, and describe how a patient could have an INCREASED AFTERLOAD with a NORMAL ARTERIAL PRESSURE: Tension = (Pressure * radius)/(wall thickness). Preload is when the chamber size is increased and the wall thickness is decreased (due to stretch) and the chamber pressure is increased prior to contraction. Afterload is when the chamber radius and wall thickness (before remodeling takes place) is not necessarily increased yet the chamber pressure is increased during contraction.
It is possible to have an increased afterload with a normal arterial pressure when you have an aortic stenosis. The heart muscle has to contract harder (increased afterload) to eject the normal amount of blood (SV) to create the normal arterial pressure.
compare and contrast the different patterns of VENTRICULAR REMODELING and
HYPERTROPHY seen with:
INCREASED PRELOAD (volume loading): On X-ray the heart is
concentric. The pressure in the chamber has increased so to help normalize
the Tension, the heart increases the wall thickness without increasing the
chamber radius significantly.
INCREASED AFTERLOAD (pressure loading): On X-ray the heart is eccentric. The extra flow of blood into the heart has increased the tension. The heart in order to help normalize the tension increases the chamber radius without significantly increasing (or decreasing) the wall thickness.
demonstrate an understanding of the role of ADENOSINE, ENDOTHELIN, and
EDRF in the local autoregulation of coronary blood flow and in the MATCHING OF
CORONARY PERFUSION AND MYOCARDIAL OXYGEN DEMAND:
Adenosine: In the presence of very low concentrations of oxygen
in the muscle cells, a large proportion of the cell's ATP degrades to adenosine
monophosphate, then small portions of this are further degraded to release
adenosine into the tissue fluids of the heart muscle. Adenosine is the
substance with the greatest vasodilator propensity. Guyton 258
This vasodilation makes it easier for blood to flow into the coronary arteries
during diastole.
Endothelin: ??? Ask Dr. Norton
EDRF: ??? Ask Dr. Norton
compare and contrast in words or by using a chart the RELATIVE IMPORTANCE
OF MECHANICAL, METABOLIC, AND NEUROHUMORAL FACTORS in the overall control of
blood flow through the coronary circulatory bed:
Mechanical: Do to the fact that coronary arteries lie in the
cardiac muscles it is important to note that blood flow for the most part stops
during systole and only flows during diastole. The coronary arteries get
compressed during systole and are occluded.
Metabolic: The main reason for dilation of coronary arteries.
They locally dilate r/t metabolic substances (high CO2, H+,
adenosine etc).
Neurohumoral: The main neural receptors that are available are
alpha 1 & 2 and beta 2. On stimulation of these receptors, the
coronary arteries both dilate and constrict...but mostly constrict.